Why women can’t afford to ignore their heart health — and how to spot the warning signs before it’s too late.

Introduction: The Hidden Threat No One Talks About Enough
If you ask most people what they think is the number one health threat to women, many will answer breast cancer. It’s understandable — decades of awareness campaigns, pink ribbons, and charity walks have etched that message into our collective consciousness.
But here’s the truth that’s far less publicized: heart disease is the leading cause of death among women worldwide. It claims more lives than all cancers combined — and yet, many women still see it as a “man’s disease” or something to worry about only later in life.
That dangerous misconception means many women don’t recognize early warning signs, don’t get screened, and sometimes don’t act quickly when symptoms appear.
The reality? Heart disease in women often presents differently than in men, and those differences can make it harder to detect — sometimes until it’s too late. This is why it’s called the silent killer.
Understanding Heart Disease in Women

Heart disease is an umbrella term for several conditions that affect how the heart works, including:
- Coronary artery disease (CAD) — when the arteries that supply the heart muscle become narrowed or blocked by plaque buildup.
- Arrhythmias — irregular heart rhythms that can interfere with efficient pumping.
- Heart failure — when the heart can’t pump enough blood to meet the body’s needs.
- Heart valve problems — where valves don’t open or close properly, affecting blood flow.
While these conditions also affect men, research has shown that women’s hearts can develop disease differently — and that hormonal, anatomical, and even microvascular (tiny vessel) differences play a role.
Why Women’s Symptoms Can Be Overlooked
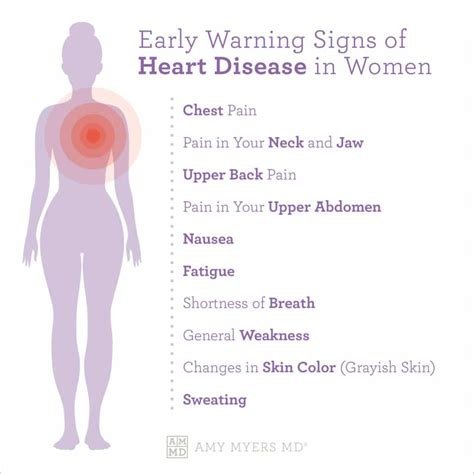
The classic heart attack symptom most of us picture — crushing chest pain that radiates to the left arm — is more common in men. Women may have chest discomfort, but often their symptoms are less obvious, such as:
- Unusual fatigue (sometimes days or weeks before the event)
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or dizziness
- Discomfort in the jaw, neck, shoulder, upper back, or upper belly
Because these symptoms can mimic less serious issues — like indigestion, stress, or a muscle strain — women sometimes dismiss them, or doctors may not immediately suspect heart trouble.
The Role of Risk Factors in Women’s Heart Health
Some risk factors are shared between men and women:
- High blood pressure
- High cholesterol
- Diabetes
- Smoking
- Obesity
- Family history of heart disease
But women also face unique or under-recognized risk factors, including:
- Pregnancy-related complications (gestational diabetes, preeclampsia)
- Autoimmune diseases (more common in women)
- Menopause (loss of estrogen’s protective effect)
- Depression and chronic stress (both linked to higher cardiac risk)
These differences make it even more important for women to have personalized risk assessments and regular screenings.
The Silence in Awareness Campaigns
While public health efforts around heart disease have improved, most campaigns are still gender-neutral — meaning they don’t highlight the specific ways heart disease affects women. This lack of targeted messaging can leave gaps in understanding and prevention.
Social media trends, community campaigns, and grassroots organizations are starting to change this by focusing on women-specific awareness, but much more work is needed.
The Emotional Barrier: “It Won’t Happen to Me”
Another challenge is mindset. Many women prioritize family, work, and caregiving responsibilities above their own health. They might delay going to the doctor or ignore symptoms because they “don’t have time” — or because they assume something less serious is going on.
But the statistics are sobering:
- 1 in 3 women will die from cardiovascular disease.
- Women are more likely to die within a year of a heart attack compared to men.
- Delays in treatment significantly increase mortality risk.
How to Break the Silence: Practical Steps for Women
While you can’t change your genetics, there’s a lot you can do to know your heart and protect it:
- Know your numbers: Blood pressure, cholesterol, blood sugar, BMI.
- Learn your family history: It’s one of the most important predictors of risk.
- Recognize women’s symptoms: Fatigue, shortness of breath, nausea, jaw/back pain.
- Don’t ignore your gut: If something feels off, get checked — even if it’s “just in case.”
Schedule regular check-ups: Prevention works best before problems start.
Real-Life Story: Maria’s Wake-Up Call
Maria, a 48-year-old mother of two, thought her tiredness was just part of a busy life. She also had some stomach upset and mild back pain but didn’t connect it to her heart.
When she nearly fainted while grocery shopping, her husband insisted they go to the ER. Tests revealed she was having a heart attack. Doctors said getting help when she did probably saved her life — but earlier recognition could have prevented the attack altogether.
Maria now shares her story online to remind women: “Your life is worth the appointment. Don’t brush it off.”
The Future of Women’s Heart Health
Advances in wearable health technology, increased use of personalized medicine, and community awareness campaigns are making it easier for women to monitor their heart health and catch problems early.
But the most important change will come from women taking their symptoms seriously and healthcare systems listening more closely when women describe their concerns.
Takeaway: Your Heart Deserves the Same Care You Give Others
Heart disease doesn’t have to be a silent killer. The more you know about the ways it shows up in women — and the more you act on that knowledge — the better your chances of living a long, heart-healthy life.
If you ever feel uncertain about your symptoms, don’t wait. Your future self will thank you for making the time to get checked.
References
- U.S. National Heart, Lung, and Blood Institute – Heart Disease in Women.
- Centers for Disease Control and Prevention – Women and Heart Disease Facts.
- Harvard Medical School – Heart Disease: A Woman’s Problem.
Disclaimer
This article is for educational purposes only and is not a substitute for professional medical advice. If you think you may be experiencing heart-related symptoms, seek immediate medical attention.